-
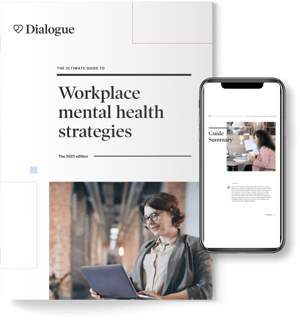
Integrated Health Platform
Overview
-
Integrated Health Platform
Improve the overall health and wellness of your organization with a single, modern platform.
-
How we're different
We drive real member outcomes through virtual care and Humanized Healthcare.
-
Our clients
Improve productivity, reduce absenteeism, and build a culture of happiness and well-being.
Programs
-
 Employee Assistance Program
Employee Assistance Program
Essential wellness services to stay happy and healthy, in one digital-first platform.
-
 Mental Health+
Mental Health+
Flexible, integrated, and personalized mental health care, backed by science.
-
 Primary Care
Primary Care
A complete member journey accessible from our industry-leading virtual care platform.
-
 Wellness
Wellness
Empower all of your members to proactively adopt healthy habits.
Features
-
Women's and Family Health
We’re spotlighting women’s health stories and unveiling something big.
-
EAP cost savings calculator
Measure what matters with Dialogue's EAP Cost Saving Calculator
-
 The business case for virtual mental health care
The business case for virtual mental health care
This is the cost-benefit analysis your leadership team needs to see.
-
-
Why Dialogue
Dialogue Experience
-
For organizational leaders
Discover how we can help drive positive outcomes for your organization.
-
For partners
Elevating Canadians’ healthcare expectations, together.
-
For members
Members can expect a better experience compared to traditional employee benefits and care.
-
 Healthiest Workplace Awards
Healthiest Workplace Awards
Recognizing Canada’s top organizations leading the way in employee health and well-being.
Why Dialogue
-
 Discover your savings
Discover your savings
High-quality, virtual benefits for your employees aren’t an expense - but an investment
-
Why virtual care?
Explore the positive impact of Dialogue's virtual care.
-
Ultimate Guide to EAP
Learn how Dialogue is reinventing the EAP experience.
-
About us
Dialogue is the leading health and wellness provider in Canada.
-
-
Resources
Learn
-
Resources centre
Discover the latest news, content and reports for HR leaders.
-
Blog
Learn more about health, organizational well-being, and life at Dialogue!
-
Case studies
Learn how we improve the health and wellness of our clients.
-
 Newsletter
Newsletter
Stay a step ahead on employee benefits, wellness, and productivity news and resources.
Support
Overview
13x the ROI: The business case for virtual mental health care
Download the reportEconomists modelled the true cost of untreated mental health and found a clear solution for employers.
2026 Healthiest Workplace Awards
Discover the awardsSee the official rankings of Canada’s top 120 workplaces, setting the standard for team well-being.
The cost of neglecting women’s health
Watch the recordingWe’re spotlighting women’s health stories and unveiling something big.
-
-
Get Pricing




 Canada (EN)
Canada (EN)
 Global (EN)
Global (EN)


































.png)

.png)

%201-1.jpg)
%202.jpg)


.jpg)



.jpg)


%204.jpg)
%205.jpg)


-1.png)

%206.jpg)
%206%20(2).jpg)
%206%20(1).jpg)


-1.png)

.png)